Sciatica Massage Therapy by Robert Pineau, LMT
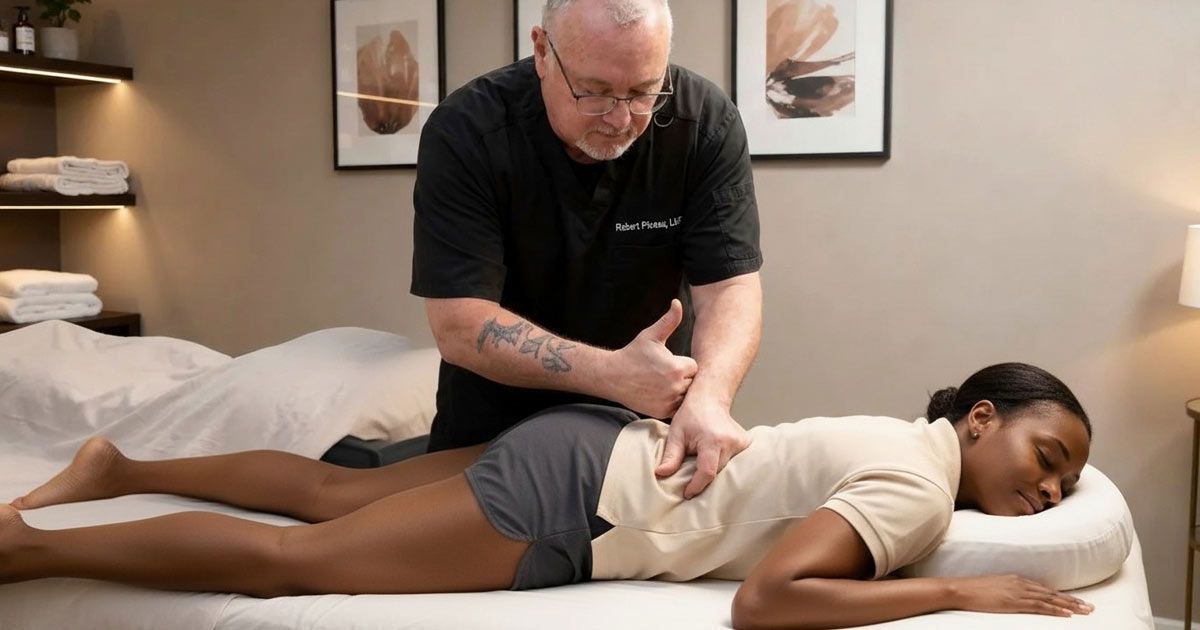
Sometimes it feels like you're walking through a mine field. I understand how deeply Sciatica and sciatic nerve pain can interfere with your comfort, mobility, and overall quality of life, and I want you to know that you’re not alone in what you’re feeling. As a Licensed Massage Therapist in the top 1% of my field, I’m here to support the root causes of your symptoms and help you move with greater ease and confidence.
-Robert Pineau, LMT
Sciatic Pain Relief by Massage Therapist Robert Pineau. Serving Patients with In‑Home Sessions or Treatments at My Massage Therapy Practice in Ronkonkoma, Suffolk County
What Is Sciatica?
Sciatica is a nerve‑related pain pattern that occurs when the sciatic nerve becomes compressed, irritated, or inflamed along its pathway from the lower back down the legs. This discomfort can range from mild tingling to severe, radiating pain that disrupts daily activities. Many patients describe it as sharp, burning, or electric-like sensations that worsen with sitting, bending, or standing for long periods. Sciatica can also create muscle tightness, weakness, or numbness in the lower body.
Sciatic nerve pain often develops gradually but can intensify quickly if the underlying cause is not supported. While Sciatica is commonly associated with lower back issues, it can also stem from hip, pelvic, or muscular imbalances. Understanding the nature of sciatic nerve irritation helps guide the most effective supportive strategies. My role is to help reduce nerve compression, improve mobility, and support long‑term comfort.
Types of Sciatic Pain
Sciatica can show up in different ways depending on the source of nerve irritation, and understanding these variations helps patients recognize what they’re experiencing. Each type affects the body differently and may influence how symptoms progress over time.
- Acute Sciatica — This form appears suddenly, often after lifting, twisting, or prolonged sitting. Symptoms can be intense but may improve with proper support and reduced nerve compression.
- Chronic Sciatica — Chronic Sciatica lasts longer than 12 weeks and may fluctuate in severity. Patients often experience recurring flare‑ups that impact mobility and daily routines.
- Alternating Sciatica — Pain switches from one leg to the other, often due to pelvic instability or sacroiliac joint imbalance. This pattern can make walking or standing feel unpredictable.
- Bilateral Sciatica — Both legs are affected at the same time, typically from central spinal compression or structural issues. This type can significantly impact posture and movement.
- Sciatica from Piriformis Syndrome — The piriformis muscle compresses the sciatic nerve, causing deep gluteal pain and radiating leg discomfort. Symptoms often worsen with sitting or climbing stairs.
- Sciatica from Herniated or Bulging Discs — Disc pressure on the sciatic nerve creates sharp, radiating pain down the leg. Patients may also experience numbness, tingling, or weakness.
- Sciatica from Spinal Stenosis — Narrowing of the spinal canal compresses the nerve roots, leading to pain that increases with standing or walking. Sitting may temporarily ease symptoms.
- Sciatica from Muscle Imbalances — Tight or weakened muscles in the hips, glutes, or lower back can pull the pelvis out of alignment, irritating the sciatic nerve. This type often develops gradually.
Sciatica can present in many forms, and each variation requires a supportive approach that focuses on reducing nerve irritation and restoring mobility. Understanding your specific pattern helps me tailor sessions that address the root cause and promote long‑term comfort.
Common Causes of Sciatica
Sciatica can develop from a variety of structural, muscular, and lifestyle‑related factors. Herniated or bulging discs are among the most common causes, placing pressure on the sciatic nerve roots. Degenerative disc changes can also narrow the spaces where nerves exit the spine, increasing irritation. Muscle tightness in the piriformis, glutes, or hamstrings can compress the nerve and trigger radiating pain. Poor posture, prolonged sitting, or repetitive movements may strain the lower back and contribute to nerve irritation.
Pregnancy can shift pelvic alignment and increase pressure on the sciatic nerve. Spinal stenosis, arthritis, or bone spurs may also reduce nerve space and create discomfort. Even stress‑related muscle tension can intensify symptoms. Understanding the underlying cause helps guide supportive strategies that reduce nerve compression and improve mobility.
Common Sciatica Symptoms
Sciatica symptoms can vary widely, but most patients experience a combination of nerve‑related sensations and muscular discomfort. These symptoms often interfere with walking, sitting, sleeping, and daily activities.
- Radiating Leg Pain — Pain travels from the lower back or glute down the leg, often reaching the calf or foot. This discomfort may feel sharp, burning, or electric-like and can worsen with movement.
- Numbness or Tingling — Patients may feel pins-and-needles sensations along the nerve pathway. These sensations often appear in the thigh, calf, or foot and may come and go throughout the day.
- Lower Back Pain — Aching or stiffness in the lumbar region often accompanies sciatic nerve irritation. This discomfort may intensify with bending, lifting, or prolonged sitting.
- Muscle Weakness — The affected leg may feel unstable or fatigued, especially during walking or climbing stairs. Weakness can develop gradually as nerve irritation persists.
- Hip or Glute Tightness — Deep pressure or tightness in the hip or glute muscles can signal nerve compression. This discomfort may worsen when sitting or transitioning from sitting to standing.
- Difficulty Standing or Walking — Pain may increase with weight-bearing activities, making movement feel restricted. Some patients experience relief only when lying down.
Sciatica symptoms can disrupt daily routines and significantly impact comfort and mobility. Recognizing these signs early allows for supportive strategies that reduce nerve irritation and promote long‑term relief.
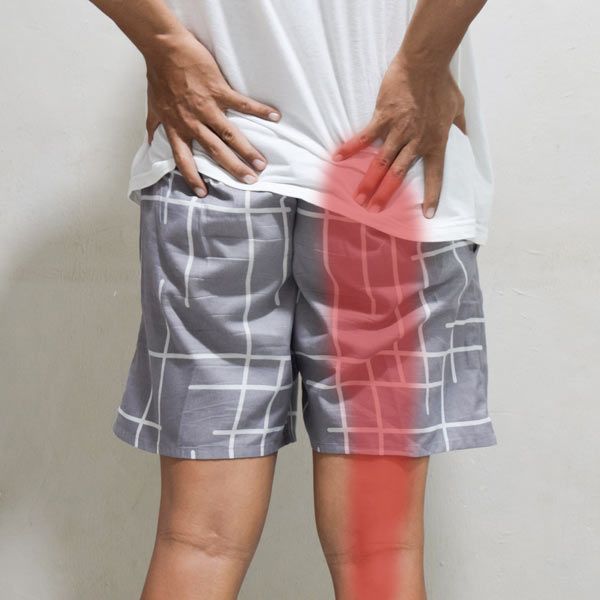
Candidates for Massage Therapy for Sciatica by Robert Pineau, LMT
Patients who experience radiating leg pain, numbness, or tingling along the sciatic nerve pathway may benefit from supportive massage therapy. Individuals with muscle tightness in the glutes, hips, or lower back often respond well to techniques that reduce nerve compression. Those who sit for long periods, perform repetitive movements, or engage in physically demanding work may also be strong candidates. Patients with posture imbalances or pelvic misalignment frequently find that targeted massage helps restore mobility.
Individuals recovering from flare‑ups or chronic discomfort may benefit from ongoing supportive care. Pregnant patients experiencing sciatic nerve pressure can also receive safe, modified techniques. Patients who prefer a natural, hands‑on approach to supporting nerve irritation often choose massage therapy. My goal is to help each patient feel more comfortable, mobile, and confident in their daily activities.
Related Medical Conditions That Can Be Supported with Massage Therapy
Several conditions can contribute to or worsen Sciatica, and supporting these underlying issues can help reduce nerve irritation. Many patients experience overlapping symptoms that benefit from targeted massage therapy.
- Piriformis Syndrome — Tightness in the piriformis muscle compresses the sciatic nerve, causing deep gluteal pain and radiating leg discomfort. Massage helps reduce muscular tension and improve nerve mobility.
- Herniated Discs — Disc pressure on the nerve roots can create sharp, radiating pain. Massage supports surrounding muscles, reducing strain on the affected area.
- Degenerative Disc Disease — Age‑related disc changes can narrow nerve spaces and increase irritation. Massage helps improve circulation and reduce muscular compensation patterns.
- Spinal Stenosis — Narrowing of the spinal canal compresses nerve roots, leading to pain and mobility challenges. Massage supports surrounding tissues to ease tension.
- Sacroiliac Joint Dysfunction — Misalignment or inflammation in the SI joint can mimic or worsen sciatic pain. Massage helps restore balance and reduce compensatory muscle tightness.
- Hip Bursitis — Inflammation around the hip joint can contribute to nerve irritation. Massage supports surrounding muscles to reduce pressure on the area.
- Muscle Imbalances — Tight or weakened muscles in the hips, glutes, or lower back can pull the pelvis out of alignment. Massage helps restore balance and reduce nerve compression.
Supporting these related conditions helps reduce overall strain on the sciatic nerve and promotes long‑term comfort. Addressing the full picture of a patient’s symptoms leads to more effective and lasting results.
Massage Modalities That Support Patients with Sciatica
Sciatica can create deep muscular tension, nerve irritation, and mobility limitations that affect the lower back, hips, and legs. Massage therapy plays an important role in reducing pressure around the sciatic nerve and supporting healthier movement patterns. Each modality below focuses on easing muscular compression, improving circulation, and helping the body function with greater comfort. These approaches are especially helpful for patients experiencing radiating leg pain, numbness, or tightness in the glutes and lower back.
- Deep Tissue Massage — This modality focuses on the deeper layers of muscle and connective tissue that often tighten around the sciatic nerve. By easing chronic tension in the glutes, hamstrings, and lumbar muscles, Deep Tissue Massage helps reduce nerve compression and supports improved mobility.
- Myofascial Release — Myofascial Release gently softens and lengthens the fascia surrounding the hips, pelvis, and lower back. This technique helps reduce restrictions that may be contributing to nerve irritation, allowing the sciatic nerve to glide more freely.
- Neuromuscular Therapy (Trigger Point Work) — Trigger points in the piriformis, gluteus medius, and lower back can mimic or worsen sciatic pain. Neuromuscular Therapy helps deactivate these points, reducing referred pain patterns and restoring healthier muscle function.
- Swedish Massage for Circulation Support — Swedish techniques help calm the nervous system, reduce inflammation, and improve blood flow to irritated tissues. This is ideal for patients experiencing acute flare‑ups or heightened sensitivity.
- Positional Release Therapy — This gentle method places the body in positions that reduce strain on irritated tissues, helping muscles reset without deep pressure. It’s especially helpful for patients who cannot tolerate intense work due to nerve sensitivity.
- Integrated Manual Therapy — This approach blends stretching, mobilization, and soft‑tissue techniques to support the full sciatic nerve pathway. It is well‑suited for patients with long‑standing or complex symptoms involving multiple muscle groups.
Massage therapy can be a powerful supportive tool for patients experiencing Sciatica or sciatic nerve discomfort. By reducing muscular tension, improving circulation, and easing nerve compression, these modalities help patients move with greater comfort and confidence. Each technique can be tailored to the patient’s sensitivity level, symptom pattern, and overall goals for mobility and relief.
What Can Happen if Sciatica Is Left Untreated?
When Sciatica is left unaddressed, symptoms can intensify and become more persistent over time. Radiating pain may become more frequent, making daily activities increasingly difficult. Muscle weakness can develop as nerve irritation continues, affecting balance and mobility. Chronic inflammation may lead to long‑term nerve sensitivity. Postural changes may occur as the body compensates for discomfort, creating additional strain on the hips, back, and legs. Sleep quality may decline due to ongoing pain or discomfort. Patients may also experience reduced flexibility and limited range of motion. Addressing Sciatica early helps prevent these long‑term challenges and supports overall functional health.
Patient Case Study
Maribel, a 47‑year‑old woman, came to my Ronkonkoma practice experiencing sharp, radiating pain down her left leg that had been worsening for months. She described difficulty sitting at work and frequent numbness in her calf. During her assessment, I identified significant tension in her glutes, hamstrings, and lower back, along with pelvic imbalance contributing to nerve irritation. Maribel chose to receive In‑Home Sessions, as getting in and out of the car was uncomfortable for her.
Her sessions focused on reducing muscular compression around the sciatic nerve and improving mobility in the hips and lower back. She began noticing reduced tingling and improved comfort when sitting. Her walking stride became smoother, and she reported fewer flare‑ups during her workday. As her symptoms decreased, she regained confidence in her movement and daily activities. Maribel shared that she felt more in control of her body and less fearful of sudden pain. Her progress highlights how targeted, supportive massage therapy can make a meaningful difference in a patient’s quality of life.
Why Patients Choose Robert Pineau, LMT for Sciatic Pain Massage Therapy
Patients choose me because I combine advanced clinical training with a patient‑centered approach that focuses on the root causes of sciatic nerve irritation. My top 1% training allows me to understand the complex muscular and structural patterns that contribute to Sciatica. I take time to listen to each patient’s symptoms, lifestyle, and goals to create a supportive plan tailored to their needs.
Many patients appreciate my ability to identify subtle imbalances that may be contributing to their discomfort. I offer both In‑Home Sessions and office visits, giving patients flexibility based on their comfort and mobility. My techniques are designed to reduce nerve compression, improve circulation, and restore functional movement. Patients value the calm, supportive environment I create during each session. My goal is always to help patients feel more comfortable, mobile, and confident in their daily lives.
Frequently Asked Questions for Sciatic Massage Therapy
- Can Sciatica improve even if symptoms have been present for years? - Many patients with long‑standing Sciatica experience meaningful improvement when nerve compression and muscular tension are properly supported.
- Why does Sciatica feel worse when sitting? - Sitting can increase pressure on the lower back, hips, and glutes, which may compress the sciatic nerve and intensify symptoms.
- Can Sciatica cause symptoms in only part of the leg? - Yes, depending on which portion of the nerve is irritated, symptoms may appear in the thigh, calf, or foot.
- Is Sciatica always caused by a spinal issue? - No, muscular imbalances, pelvic alignment issues, and hip tension can also contribute to sciatic nerve irritation.
- Can massage therapy help prevent Sciatica flare‑ups? - Regular supportive sessions can help maintain mobility, reduce muscular tension, and minimize factors that contribute to nerve irritation.
Contact Robert Pineau, LMT for a Free Sciatica Massage Therapy Consultation in Ronkonkoma, Suffolk County
If you’re experiencing Sciatica or sciatic nerve discomfort, I’m here to help you feel supported, understood, and guided toward greater comfort. My approach focuses on reducing nerve compression, improving mobility, and addressing the root causes of your symptoms. Whether you prefer In‑Home Sessions or visiting my Ronkonkoma practice, I’ll create a supportive plan tailored to your needs. Contact me today to schedule your free consultation and begin your path toward improved comfort and confidence.
Please contact us today.
Additional References
- Low Back Pain Fact Sheet - National Institute of Neurological Disorders and Stroke (NINDS)
- Sciatica - U.S. National Library of Medicine – MedlinePlus






